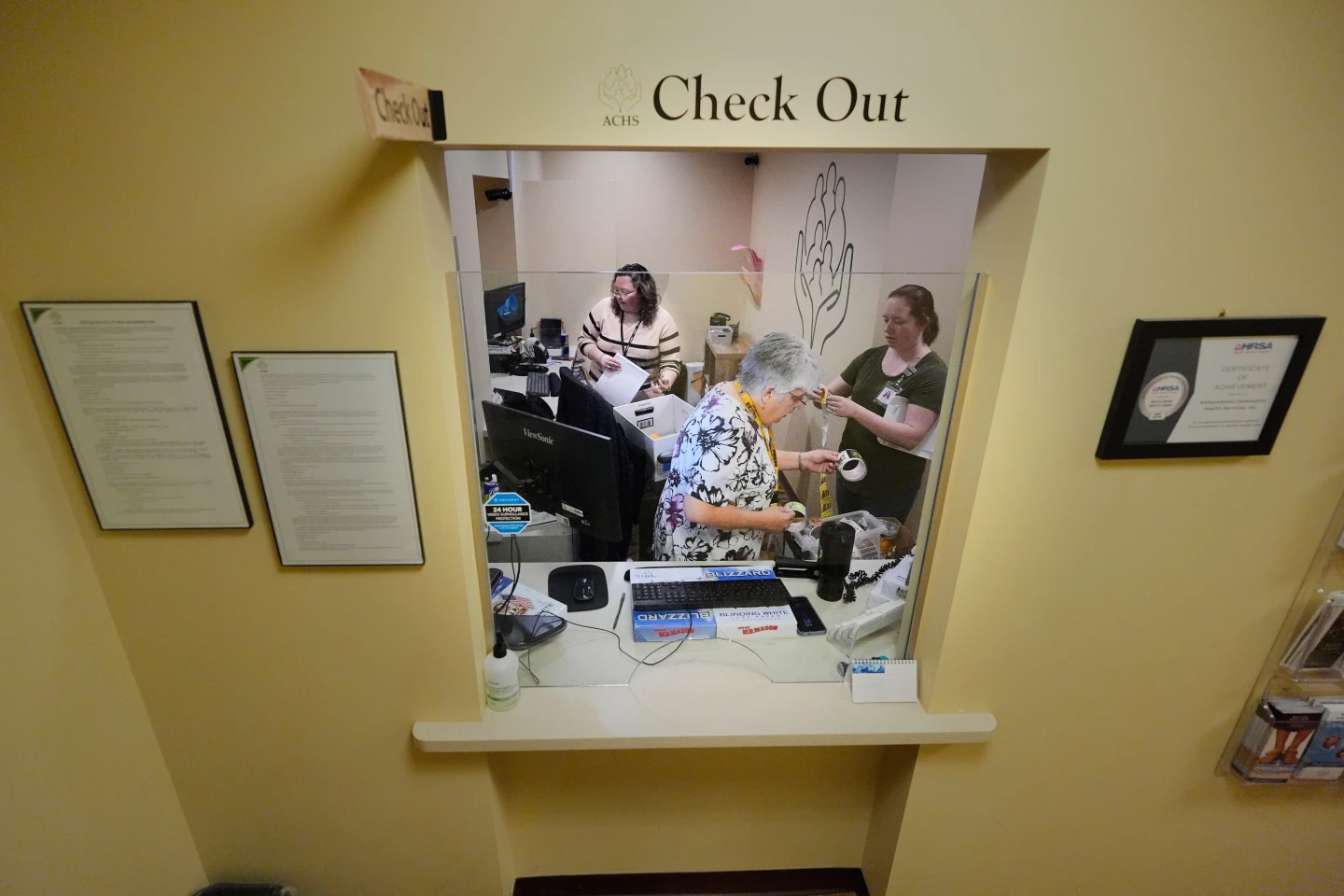
FRANCONIA, NH — For over twenty years, Susan Bushby, a 70-year-old housekeeper from the picturesque town in New Hampshire's White Mountains, found solace in her local community health center. Known for its warm atmosphere and familiar staff, this medical building served as a second home for Bushby and many others.
However, the site of the Ammonoosuc Community Health Services closed its doors last month, compelling patients to travel at least ten miles to access another health center, which stirs anger and heartbreak among locals who relied on the familiar faces and care.
“I was very disturbed. I was downright angry,” shared Bushby, shedding tears as she reflected on leaving behind trusted medical professionals and the comforting environment. “It’s really hard for me to explain, but it’s going to be sad.”
The closure raises pressing concerns, as officials attribute it to significant cuts in Medicaid. Nearly half of the 1,400 patients are elderly, many facing severe health challenges, with the nearest alternative medical facility inaccessible to those with limited mobility. Local residents like Marsha Luce worry about deteriorating health outcomes as they lose their close-knit health community.
“It’s going to be hard,” Luce stressed, deeply concerned about the continuity of care and personal relationships cultivated over the years. “A lot of families have come to rely on this place. It’s not just about health care; it’s about relationships.”
Implications for Rural Health Care
The closure of the Franconia center resonates with a broader trend impacting rural healthcare facilities across the United States. Over 100 hospitals have shut down in the past decade, with an alarming number at risk due to financial instability stemming from Medicaid cuts and rising insurance premiums.
“These Medicaid cuts are going to hit rural hospitals hard,” voiced New Hampshire Senator Maggie Hassan. “Providers are seeing more patients without insurance, leading to increasingly tough decisions.”
Ed Shanshala, CEO of Ammonoosuc, recognized the severity of the situation after recent legislation cut over $2 million in federal funding across their network. With finances already tight, he resorted to closing down operations in Franconia to maintain their remaining health centers.
“We’re left with no choice,” he noted, regretting the emotional toll on both staff and patients as the center dismantled its operations without a proper farewell. “It’s devastating on a relational level.”
The ongoing closure has sparked an urgent dialogue regarding the future of healthcare access in rural regions. Residents like Jill Brewer, a local leader, express anxiety that this might be the start of a cascading failure in rural health systems.
On the final day, the atmosphere was somber, highlighting the intense emotional strain this closure has thrust on a rural community that thrives on connection and trusted care.